Download PDF
RCA TRAINING
Root Cause Analysis training by Sologic provides the tools, skills, and knowledge necessary to solve complex problems in any sector, within any discipline, and of any scale. Learn MoreSOFTWARE
Sologic’s Causelink has the right root cause analysis software product for you and your organization. Single users may choose to install the software locally or utilize the cloud. Our flagship Enterprise-scale software is delivered On Premise or as SaaS in the cloud. Learn MoreRecently an MRI center experienced a near-miss event when a ferrous oxygen bottle was pulled into the magnetic bore of an MRI machine. The patient and staff were present in the magnet room at the time of the event, although not in the line of fire between the oxygen cylinder and the magnet. They were also exposed to helium gas released when a staff member initiated emergency shutdown of the magnet. A risk assessment determined that this was a potentially catastrophic (SAC Matrix score = 3) event, which could have resulted in serious injury and/or fatality.
Summary of Solutions*:
*Detailed solutions listed below
Stronger Actions:
- Reconfigure the existing space to best reduce risk of ferrous object intrusion.
- Visibly mark site-supplied, non-ferrous oxygen bottles.
- Install a ferrous metal detection device.
- Acquire professional MRI safety expertise.
- Retrofit the facility to include supplied oxygen.
Intermediate Actions:
- Develop/modify the pre-admission checklist that includes consideration of patient-supplied oxygen and whether or not it is needed during the MRI procedure.
- Upon arrival, assess all patient belongs and ensure that all ferrous materials are declared.
- Flag patients in the system who require supplied oxygen. Replace all patient-supplied oxygen bottles with marked site-supplied non-ferrous bottles.
- Proactively address risks of increasing the number of scans.
- Peg production levels to staffing. Develop a safe patient/staff ratio.
- Obtain MRI emergency training, including periodic drills.
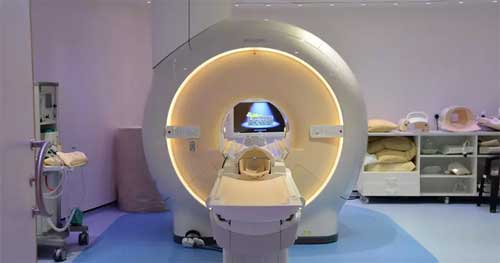
Recently an MRI center experienced a near-miss event when a ferrous oxygen bottle was pulled into the magnetic bore of an MRI machine. The patient and staff were present in the magnet room at the time of the event. They were not in the line of fire between the oxygen cylinder and the magnet, and therefore were not struck by the flying cylinder. They were also exposed to, but not injured by, helium gas released when a staff member initiated emergency shutdown (also called “quenching”) of the magnet. A risk assessment determined that this was a potentially catastrophic (SAC Matrix score = 3) event, which could have resulted in serious injury and/or fatality.
Facility Shut Down Five Days:
The staff initiated an emergency shutdown because they were concerned that the oxygen bottle would rupture or explode. This assumption was incorrect – bottle-rupture was not a risk. The staff has not been trained in MRI emergency response. No emergency drills are conducted. There is also no designated MRI Safety Officer.
The emergency shutdown damaged the MRI machine, requiring five days to repair. No scans were completed during this time.
Ferrous Oxygen Bottle Not Detected:
The patient was admitted to the magnet room with his own bottle of supplemental oxygen. This bottle was made from ferrous material. The staff utilizes a pre-scan checklist to identify ferrous items, but this list does not address supplemental oxygen bottles. The facility normally would supply non-ferrous oxygen bottles to patients for the duration of their visit, but confusion during check-in caused them to miss this one. Compounding the issue, ferrous oxygen bottles look very similar to non-ferrous bottles, which makes them difficult to visually identify. By the time the patient was ready to enter the magnet room, the staff assumed that all ferrous objects had been accounted for and removed.
There is no ferrous metal detection system in the MRI suite. The Ordering Physician did not consider whether the patient could discontinue supplemental oxygen during the MRI procedure. And the facility is not configured with four progressively safer zones per ACR recommendations. It was constructed prior to the four-zone recommendation and existing space constraints preclude it from being reconfigured.
Schedule Pressure:
The staff was very busy during the admission procedure for this patient - they were three scans behind schedule and were trying to catch up. A second MRI technician had to leave work due to illness. No additional staff was available to replace the sick technician. At the time, the facility was not meeting target quality/timeliness metrics. It has experienced a 50% increase in number of scans conducted this year. Managing this growth has proved to be challenging. This growth represents a potential systemic risk that should be examined further in a separate investigation.